Describtion
Radical Cystectomy in Female Patients
PREOPERATIVE PREPARATION AND PLANNING
There are few differences in preoperative preparation for women
facing radical cystectomy compared with men. Prior gynecologic
surgery should be noted, and when oncologically sound, discussion
regarding vaginal sparing in women who wish to remain
sexually active should be undertaken. Detailed preoperative
medical evaluation and optimization, counseling regarding urinary
diversion together with an enterostomal therapist, comprehensive
metastatic evaluation, and mitigation of thromboembolic complications
remain important aspects in women. Availability of a
sponge stick for intravaginal manipulation during dissection and
Babcock forceps for retraction of the uterus are notable additions
to the instruments required for radical cystectomy in men. Refer
to the Chapter 48 for further details on preoperative planning for
radical cystectomy.
PATIENT POSITIONING AND SURGICAL INCISION
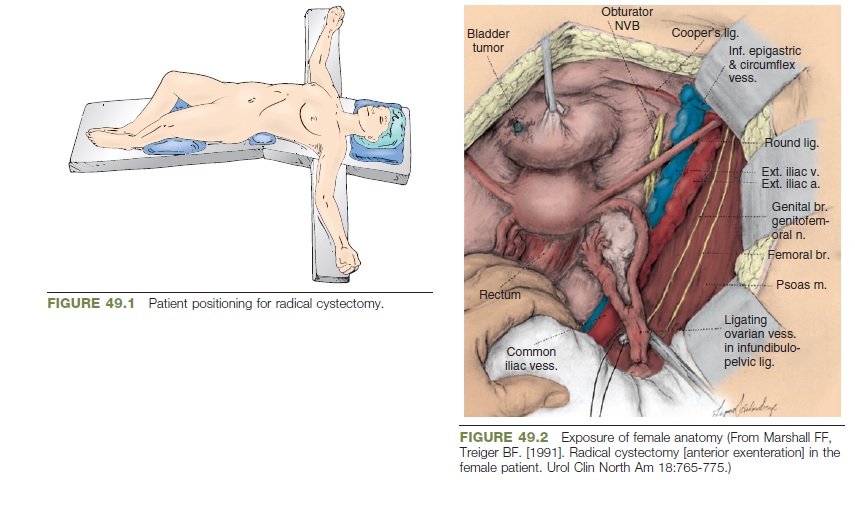
Position the patient with the umbilicus over the break in the table
in a hyperextended position using the kidney rest and flexing the
table (Fig. 49.1). To permit access to the vagina, the lower extremities
are placed in a frog-legged position with the knees wellsupported.
Alternatively, the patient may be placed into a low
dorsal lithotomy position. The skin is prepped from the nipples
to the midthigh, including a thorough vaginal prep. After draping
the abdomen, including maintaining access to the vagina, insert
an 18-Fr urethral catheter. Clip the catheter to the drapes for
accessibility throughout the case. A primary right-hand-dominant
surgeon should stand on the left side with the assistant on the
right. Make a lower midline abdominal incision from the symphysis
pubis to just below or lateral to the umbilicus.
OPERATIVE TECHNIQUE
Incise the anterior rectus fascia and the transversalis fascia. Bluntly
with a Kittner sponge stick but under direct visualization, open
the space of Retzius and establish the potential space between the
bladder and the pelvic sidewall and the external iliac vessels.
Examine the lymph nodes; if concern for disease exists and neoadjuvant
chemotherapy has not been given, proceed with lymph
node dissection and frozen section. Otherwise, lymph node dissection
can be completed after bladder removal.
Incise the peritoneum in line with the abdominal incision.
Locate, ligate, and then divide the urachus and incise the peritoneum
in a V shape, dissecting the “wings” of the bladder peritoneal
attachment. A Kocher clamp on the urachus is useful for traction
(Fig. 49.2). Assess mobility of the tumor and bladder (this should
have been assessed preoperatively as well via examination under
anesthesia and rectal examination). Explore the abdomen, palpating
especially the liver and preaortic and pelvic nodes. Release
intraabdominal adhesions at this time.
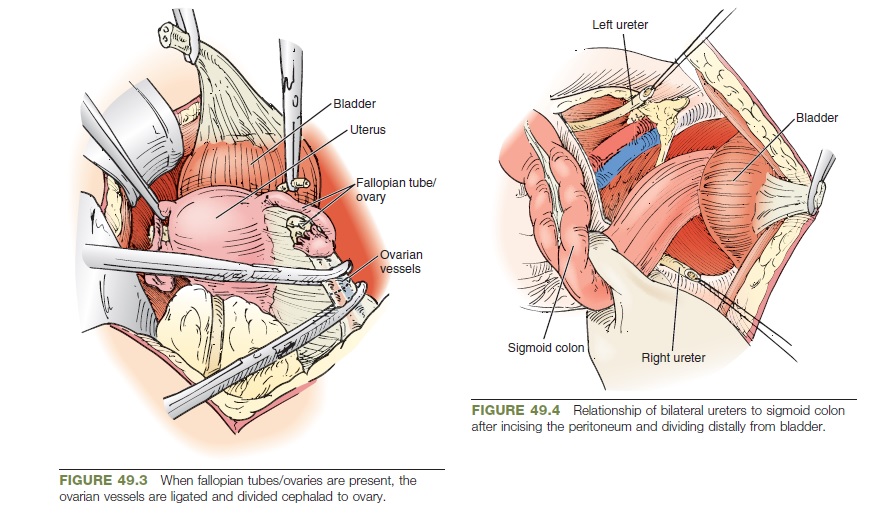
The peritoneum lateral to the bladder is incised, and the round
ligament is ligated and divided. The ovarian vessels in the infundibulopelvic
ligament are identified, ligated, and divided. Alternatively,
these vessels can be controlled with a vessel-sealing device
such as the Caiman, LigaSure, or Harmonic (Fig. 49.3).
Mobilization of Bowel and Exposure
Mobilize the sigmoid colon to allow exposure for dissection of the
left ureter. The small bowel should then be packed into the upper
abdomen using several radiopaque laparotomy towels with a symmetric
exposure of the left and right side and sigmoid colon in
the middle. The Bookwalter retractor provides excellent exposure.
Extensive mobilization of the right colon is not necessary
Identification of Ureters
A malleable blade can be used to retract the sigmoid colon to
either side when identifying and dissecting the ureters (Fig. 49.4).
On the right side, the peritoneum is incised parallel to the
common iliac vessels, and the ureter is identified as it crosses this
structure. The ureter is isolated with a vessel loop and dissected
with preservation of as much periureteral tissue as possible to
avoid devascularization. Grasping the ureteral tissue with instruments
should be avoided. The obliterated umbilical artery or
superior vesical artery is encountered as the ureter runs posteriorly.
This is ligated to help provide adequate ureteral length, and the
dissection is carried to the level of entry into the bladder. The
ureter is ligated and divided, avoiding spillage from the bladder.
If desired, frozen section biopsy can be performed. In the
setting of small ureters, the distal end can be clipped and tied to
allow for some dilatation during the remaining dissection before
urinary diversion. A tacking suture should be placed to help with
manipulation and to avoid ureteral trauma.
Dissect similarly the left ureter but continue more proximally
than on the right. When the dissection has arrived at the bladder,
transect the ureter as done previously. Under direct vision, incise
the retroperitoneum on each side of the sigmoid colon and establish
a generous opening from one retroperitoneal opening to the
other coursing under the sigmoid colon and its mesentery. This
should be done just anterior to the sacrum and, if cephalad to the
bifurcation of the aorta, anterior to the aorta. Place a McDougal
clamp or other large curved clamp and bring the ureter to the
right side. Be sure that the ureter is not twisted or kinked by the
peritoneum or vessels and that it courses in a smooth curve
through this passage.
Posterior Dissection
Using anteriorly directed traction on the uterus and concomitant
posterior and superior retraction on the rectosigmoid, excellent
exposure is provided for incision of the rectouterine pouch and
mobilization of vaginal wall off the rectosigmoid colon. The
classic anterior pelvic exenteration includes removal of the bladder,
uterus, bilateral fallopian tubes and ovaries, anterior vaginal wall,
and urethra. A povidone-iodine–soaked sponge-stick is placed in
the vagina and pushed into and upward and anteriorly to facilitate
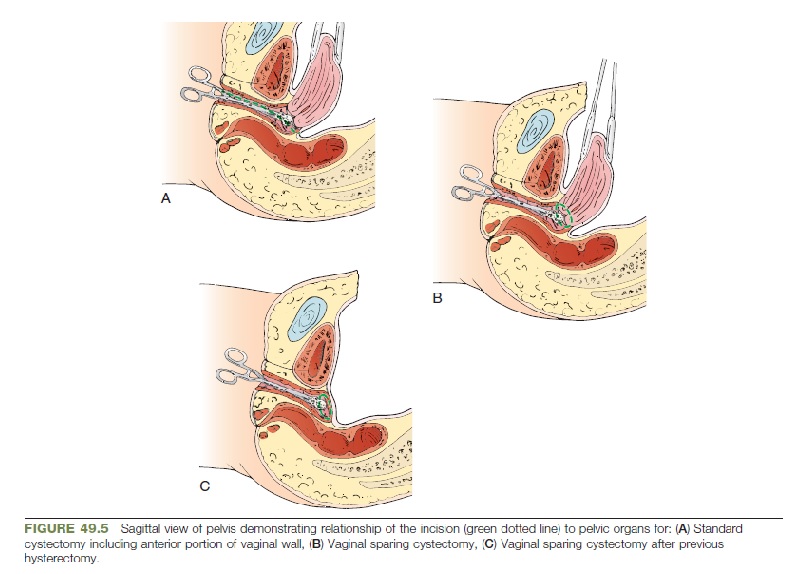
identification of the cervix at the vaginal apex. The cervix can
usually be easily palpated and using electrocautery; an incision is
made into the vagina posterior or below the cervix (Fig. 49.5).
Division of Posterolateral Pedicle
At this point, a reticulating gastrointestinal anastomosis (GIA)
stapler or vessel sealing device can be used on each side to control
and divide the posterolateral pedicles, including a portion of
anterior vaginal wall (Fig. 49.6). This is continued proceeding
distally as the bladder is retracted anteriorly up out of the incision.
If one of these devices is not available, then clear the internal iliac
artery and identify its branches. Dissecting distal to the gluteal
branch, pass a right-angle clamp gingerly behind the arterial and
venous branches, draw a 2-0 silk suture through, and ligate the
artery. Clip, tie, or suture ligate the remainder of the vesical
pedicle down to the endopelvic fascia using finger dissection to
develop the plane between the posterior bladder and the rectum.
Do not ligate the internal iliac artery.
If the primary tumor is small, resection of a large segment of
the vagina should be avoided because of the adjacent pelvic plexus
and some of the autonomic innervation that runs along its lateral
aspect. The pelvic plexus provides innervation to the smooth
muscle of the female urethra and the pudendal nerve provides
innervation to the rhabdosphincter.
Anterior Dissection and Urethral Dissection
With Urethrectomy
If urethrectomy is to be performed, the pubourethral suspensory
ligaments are identified and divided (Fig. 49.7). These are analogous
to the puboprostatic ligaments in the male. The division of
the pubourethral ligaments allows the urethra and bladder to drop
inferiorly. The dorsal vein complex can be identified and ligated.
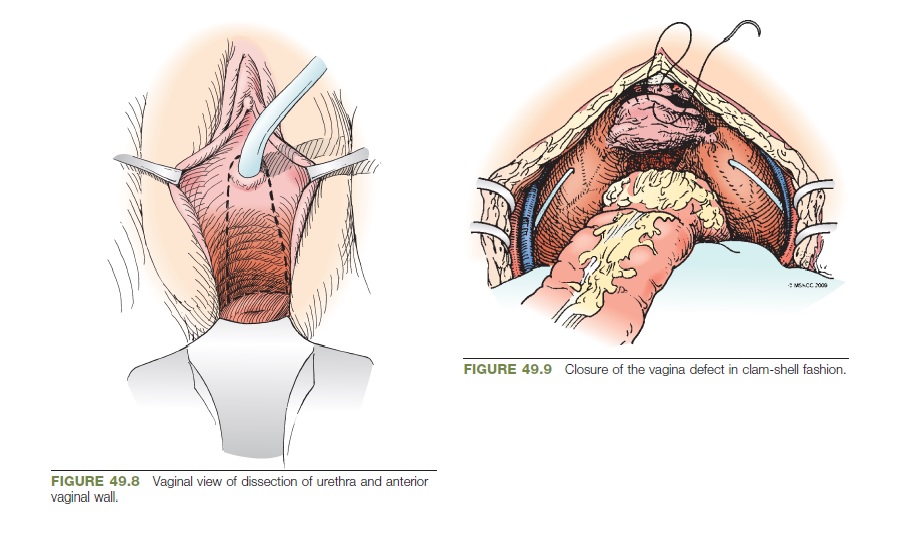
The urethra is dissected from under the dorsal vein complex so
the only remaining attachments of the specimen are the urethral
meatus and a small portion of the vagina (Fig. 49.8). The completed
specimen is passed off the table with care taken to avoid
urine spillage, and the vagina is closed (Fig. 49.9).
Vaginal-Sparing Approach
A vaginal-sparing procedure is most appropriate for patients
undergoing orthotopic urinary diversion and for patients who are
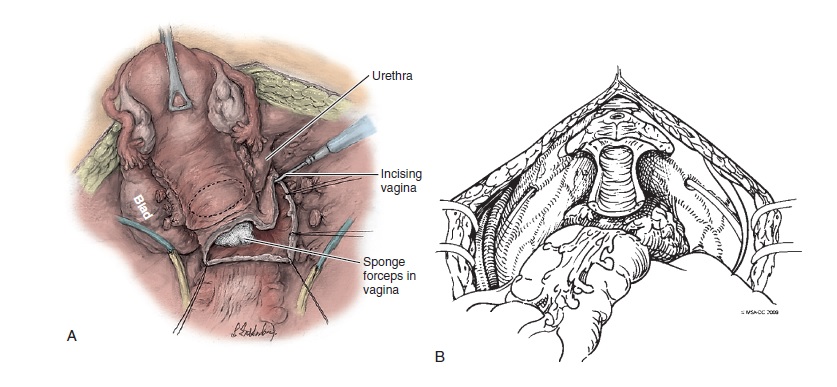
sexually active. A circumferential incision is made in the apex of
the vaginal just around the cervix (Fig. 49.5). Using countertraction
on the anterior-lateral vaginal wall, the posterior bladder is
dissected free from the anterior vaginal wall (Fig. 49.10). This
dissection is continued distally to immediately beyond the palpable
Foley balloon or the vesicourethral junction. Vaginal packing
is not routinely used but may be needed to promote hemostasis
and is removed within 24 hours of surgery.
Control of the vascular pedicles technique requires an alternative
approach and proceeds after the endopelvic fascia is well
exposed but left intact. A fat pad lying adjacent to the rectum
defines the lower limit of the lateral pedicle coursing from the
internal iliac vessels. As in men, the ureter travels below the
“bridge” of the superior vesicle artery, which can be seen and felt
with medial traction on the urachus or bladder. This is divided
and then the remainder of the small vessels can be controlled with
a Orthotopic Urinary Diversion
If a continent orthotopic diversion is being considered, only the
bladder neck and proximal 1 cm of urethra are removed (Fig.
49.11). Carefully avoiding a more extensive dissection provides
for better preservation of the muscularity and innervation of the
urethral sphincter. The dorsal vein complex can be identified and
ligated.
If results of frozen section of the urethral margin are positive,
perform urethrectomy, and orthotopic diversion should not be
performed. Otherwise, proceed with the vaginal-sparing approach
as described. If the anterior vaginal wall must be removed with
the bladder specimen, the vagina can be reconstructed, but it is
important to place interposed tissue such as an omental flap to
avoid fistula formation
. Final Steps
Check for bleeding and proceed with lymphadenectomy and urinary
diversion. After thorough irrigation, the pelvis is inspected carefully
and packed with moist laparotomy pads. If there is question
of rectal injury, an assistant can perform a rectal examination or
fill the pelvic cavity with water and instill air through a catheter
placed in the rectum to detect a leak. If the rectum is injured,
close the defect in two layers and thoroughly irrigate with antibiotic
irrigation. Consider proximal colostomy and general surgery
consult, especially in the case of prior pelvic radiation.
If there is no obvious lymphadenopathy, performing lymphadenectomy
after cystectomy facilitates a complete removal of
relevant tissue and allows for careful examination of the cystectomy
site to ensure hemostasis. After urinary diversion is performed,
carefully replace the bowel to the anatomic location after
carefully running the length. Pull the omentum down to cover
the anastomoses. An omental flap can be used to help prevent
fistula. Suction drainage is generally utilized for protection of the
diversion and to monitor for urine leak. Close the incision
appropriately.[1]
[1] Hinmans Atlas of urology surgery,Fourth edition,page 360-365
.jpg)